The field of regenerative medicine holds the promise of creating more effective treatment for damaged organ and tissues by activating the body’s natural repair system. Researchers around the globe are continually producing viable sample tissues, but there are fewer examples of effectiveness inside living organisms.
A multidisciplinary team of researchers from leading academic institutions in Japan are working on the production of a 3D bioprinted mini liver. In the most recent study, published in the journal Scientific Reports, the team demonstrates the ability to implant their 3D bioprinted liver tissue into live rats.
The successful procedure is a positive result for the further development of therapeutic treatments, and adds evidence to new ways spherical cell samples can be made.
3D is better than 2D
Many stem cell studies conclude that, when it comes to tissue engineering, 3D is better than 2D. In the case of this study from Kyushu University and partners, “The unarranged fusion of spheroids” i.e. liver cells in a 2D medium, “could not to form controlled or uniform structures.”
“Furthermore, the spheroids did not fuse at the central area due to the lack of medium supply in static culture conditions.”
And so, “To overcome these problems, we used a new 3D printing technology to create a reproducible structure and enable culture circulation.”
Pin point accuracy
Rudimentary liver buds, also called spheroids, were made into tissue by the Kenzan method of 3D bioprinting. Liver cell spheroids in the Kenzan method are placed onto an array of needles clustered close together.
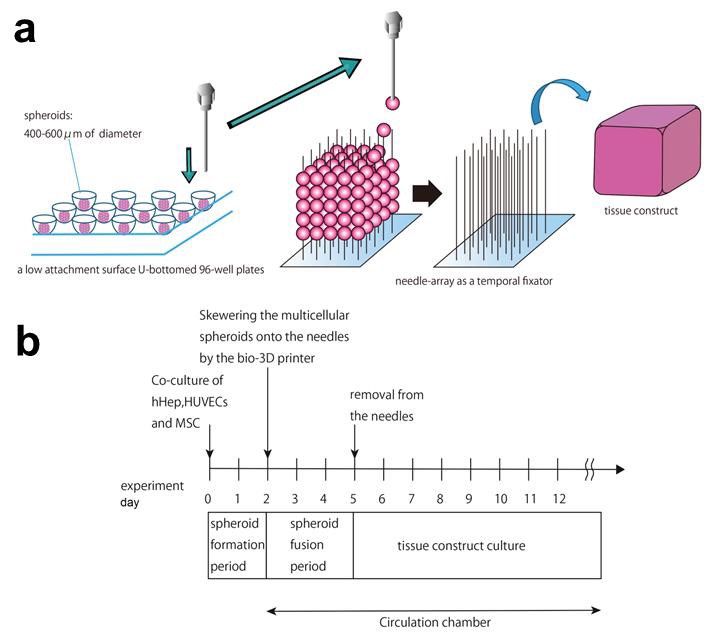
Over three days, the spheroids fuse together so they can be removed from the array. Afterwards, the sample culture closes over the holes created the needles, leaving a solid, flexible tube.
The tube shaped specimen was made from approximately 500 spheroids, and measures 4 × 4 × 5mm.
Gif shows a test of the physical strength of the 3D bioprinted liver tube. Clip via Scientific Reports, Supplementary Materials
Successful transplantation
Once fabricated the liver buds were test transplanted into living mice in a number of different ways. In the method that stood out, the 3D bioprinted sample grafted into the mouse liver in the first 7 days after transplantation. This method, according to the authors, has two major advantages. First, “it does not involve any vascular obstructions.” Second “the presence of direct connection between the graft and the recipient’s liver parenchyma” i.e. the functional part of the organ, “would facilitate greater graft growth.”
Additionally, with the Kenzan method the researchers demonstrate what they believe is both a rapid and scaleable method of making liver-like tissues. They comment, “it allows for the fabrication of elaborate geometry in 3D tissue and the fixation of the shape with the needle-array system enables the immediate execution of culture circulation after 3D printing.”

Author affiliations
The Kenzan method is commercialized by biomedical technology firm Cyfuse. Tadashi Tamura, one of the co-authors of the study is employed by Cyfuse Biomedical in a research capacity.
Other authors include Kyushu University’s Yusuke Yanagi, Tomoaki Taguchi, Koichiro Yoshimaru, Toshiharu Matsuura, Makoto Hayashida, Kenichi Kohashi, Yoshinao Oda and Takayoshi Yamaza; Shin Enosawa and Eiji Kobayashi from Keio University; and Koichi Nakayama of Saga University.
For medical research and more, like, follow, and subscribe to 3D Printing Industry. Register for 3D printing jobs here.
Featured image shows the Kenzan 3D bioprinitng and implant process as used in Kyushu University research. Image via Scientific Reports


