Researchers from Texas A&M University have combined 3D printing, biomaterial engineering and stem cell biology to create new, more efficient, customizable bone grafting materials.
Leveraging these three technologies, the scientists produced 3D printed highly-osteogenic scaffolds that not only facilitate bone cell growth but also serve as a sturdy platform for bone regeneration in custom shapes. The novel biomaterial could represent an alternative to the use of metals and polymers in reconstructive surgery, with the skin graft able to seamlessly integrate into the patient’s skull after healing.
“Materials used for craniofacial bone implants are either biologically inactive and extremely hard, like titanium, or biologically active and too soft, like biopolymers,” said Roland Kaunas, Associate Professor in the Department of Biomedical Engineering. “In our study, we have developed a synthetic polymer that is both bioactive and mechanically strong. These materials are also 3D printable, allowing custom-shaped craniofacial implants to be made that are both aesthetically pleasing and functional.”
The need for improved bone grafting technology
Each year 200,000 people suffer injuries to their jaw bone, face, or head. The resulting surgery often requires the use of titanium plates and screws to hold these broken bones in place, and to enable surrounding bone cells to grow, and form a cover around the implant. While this approach has achieved the relative success of aiding bone repair, titanium does not always integrate into bone tissue, which can then cause the implant to fail, and in advanced cases lead to further surgery.
Metals and thermoplastics are also more susceptible to infection, implant extrusion and exposure, tissue necrosis, and stress shielding compared to autologous grafts. Bone transplants are considered a preferable alternative by surgeons, but this technique has drawbacks too. Direct application of bone tissues relies on a limited source of donor tissues, incurs donor-site morbidity, and even then, complex geometries of bone in the skull cannot be easily replicated.
The researchers identified biocompatible polymers, and more specifically biogels, as a substitute for polymer and metal implants. These malleable materials are preferable because, once they are loaded with bone stem cells, the gels can be 3D printed into any pre-programmed shape. In addition, unlike metal plating, the human body can dissolve hydrogels over time, without any lasting damage.
Using 3D printed biogels to create bone transplants
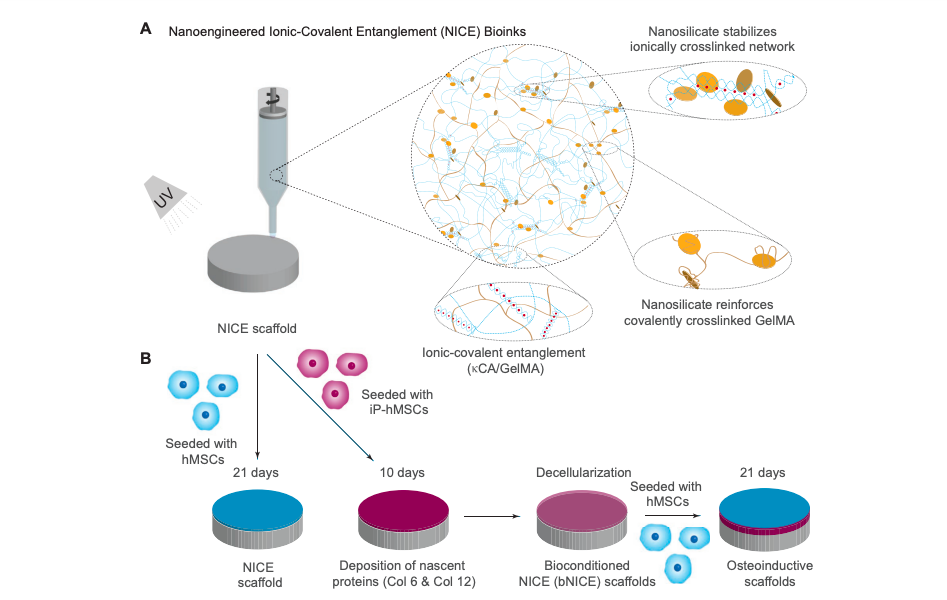
Although the pliability of biogels makes them ideal for 3D bioprinting, their flexibility also impacts on the mechanical integrity and accuracy of any parts produced. In order to make the material more rigid, the researchers developed a Nanoengineered Ionic-Covalent Entanglement or “NICE.” The recipe for this concoction includes just three main ingredients: an extract from seaweed called kappa carrageenan, gelatin, and nanosilicate particles. These elements act to stimulate bone growth and mechanically reinforce the NICE hydrogel, with the mixture found to be more than eight times stronger than its individual components.
Once the blend had been prepared, the researchers added adult stem cells to 3D parts printed with NICE ink, and then chemically induced the stem cells to convert them into bone cells. Within two weeks of the process, the scientists found that the cells had grown in numbers, producing high levels of bone-associated proteins, minerals, and other molecules. The cell secretions formed a scaffold, known as an extracellular matrix, with a unique composition of biological materials needed for the growth and survival of developing bone cells. Once the scaffolds were fully-developed, the bone cells could be removed, and the hydrogel-based implant was ready to be inserted into the site of the skull injury.
According to the researchers, the strength of the 3D printed scaffolds facilitates the attachment and growth of healthy bone cells, while allowing developing bone cells to penetrate through the synthetic material. The hydrogels are also resilient and tough, permitting manual manipulation, while also being slightly compressible, and allowing a press-fit into the defect. Due to the promising biological and physical properties of NICE grafts, the researchers are keen to use the process for bone regeneration in vivo for spinal fusion in the near future.
“Although our current work is focused on repairing skull bones, in the near future, we would like to expand this technology for not just craniomaxillofacial defects but also bone regeneration in cases of spinal fusions and other injuries,” Kaunas said.
Bone grafting in additive manufacturing
Experimental new biomaterials are a hot topic in 3D printing right now, with many academic institutions attempting to perfect the technology for bone-grafting purposes.
The university clinic Charité–Universitätsmedizin Berlin, developed 3D printed titanium-mesh scaffolds in January 2018, to offer an alternative to conventional bone-grafting techniques using a patient’s own bone. The scientists claimed that implants provided unparalleled strength, and could be designed with complex inner geometries to fit any injury.
Researchers from Connecticut-based Oxford Performance Materials (OPM) and McGill University in Canada, used 3D printed PEKK implants to accelerate bone regeneration in June 2019. The newly-devised method could aid in treatments for critical-sized bone defects, reducing the need for invasive procedures such as bone grafting.
Scientists from Rice University and the University of Maryland (UMD) developed a new proof-of-concept for 3D printed artificial bone tissue in April 2019. The cartilage was being developed to help athletes recover from sporting injuries, and those suffering from damage related to arthritis.
The researchers’ findings are detailed in their paper titled “Conditioning of 3D Printed Nanoengineered Ionic–Covalent Entanglement Scaffolds with iP-hMSCs Derived Matrix,” published in the Advanced Healthcare Materials journal. The study was co-authored by Candice Sears, Eli Mondragon, Zachary I. Richards, Nick Sears, David Chimene, Eoin P. McNeill, Carl A. Gregory, Akhilesh K. Gaharwar, and Roland Kaunas.
You can now nominate for the 2020 3D Printing Industry Awards. Cast your vote to help decide this year’s winners.
To stay up to date with the latest 3D printing news, don’t forget to subscribe to the 3D Printing Industry newsletter or follow us on Twitter or liking our page on Facebook.
Looking for a job in the additive manufacturing industry? Visit 3D Printing Jobs for a selection of roles in the industry.
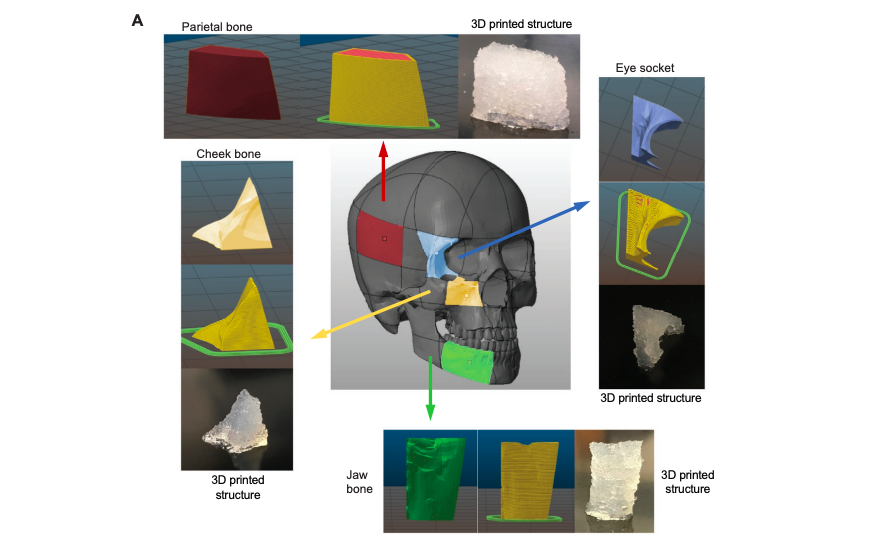
Featured image shows a 3D model of a skull, with the researcher’s biomaterial grafts inside. Photo via Texas A&M.



