Research led by biomedical lecturer Dr. Achala de Mel proposes 3D printing as an accessible approach to tissue engineering. 3D Printing Industry spoke to Dr. de Mel to understand more about the process.
By using the common method of fused deposition modeling (FDM), Dr. de Mel and her research team 3D printed a variety of plastic tubular structures that can be used to culture the building blocks of tissues found within the body.
With this approach, the researchers conceptualize a holistic approach to cell culture in labs, in opposition to dedicated facilities that drive up a costly barrier between research and patient care.
Opensource fabrication
The material focus of this study is thermoplastic polyurethane (TPU). TPU was selected for its unique malleable and elastic qualities. Though not as commonly used as PLA, TPU is widely available as a 3D printer filament and can be tailored to specific applications.
For application in medicine, this study uses a custom-made TPU. To evaluate its efficacy, two commercially available machines are used for 3D printing: the Sharebot Next Generation and Rokit 3Dison Multi, similarly priced between $1,850 and $1,990.
CAD models of the demonstrative tubes and trachea are created and sliced using Blender, Slic3r and Makerbot slicing software.

3D printed building blocks for cells
With the specially tuned TPU material, de Mel Lab researchers demonstrated the ability to rapidly fabricate a variety of different tubes. As explained in the discussion, these structures are designed as a proof of concept as, “A tubular elastic structure with varying diameter and thickness is a common structural feature of many organs”.
The infill patterns inside these tubes are designed as cell scaffolds, i.e. structures to support the growth of cells, as seen in previous 3D printing research from the likes of CWRU.
Dr. de Mel further explains the role of these structures as follows,
Scaffolds can be designed to provide cells with physical properties such as a difference in rigidity, geometries, surface roughness and anisotropy. Cells can sense these differences and respond with changes in their proliferation, differentiation as matrix synthesis ability- such responses, in-in-vivo can eventually influence physiological wellness/balance.
Commenting on the computer aided design (DAS) afforded by 3D printing, Dr. de Mel adds,
3D printing allows us to create a multiple combinations of such conditions within a scaffolds (Which is relatively not so efficient and reproducible with conventional material fabrication methods) so that we can harness a great deal of information on cell responses to 3D scaffolds – so that engineers then can chose the appropriate 3D printing design condition/s to produce scaffolds, to have intended cell responses.
3D printed tracheal models
In each tube example researchers test different sizes and infill patterns to find the one most appropriate for recreating bone porosity, therefore conducive to vascular ingrowth.

Finding rapid iterations and development of the tubes to be relatively simple to achieve, the researchers then moved on to create a model mimicking the structure of a human trachea.
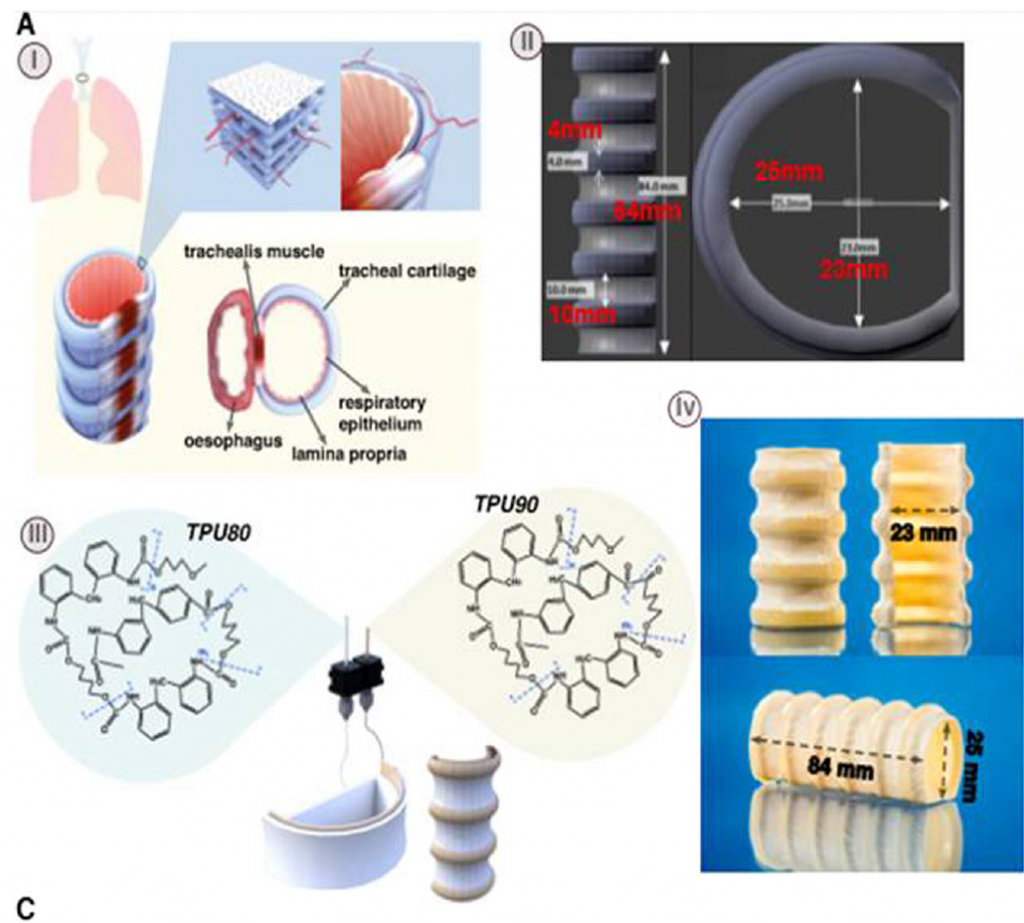
With these based structures in mind, TPU’s potential for cell culture is then put to the test in two samples: one laced with human skin cells, and the other with stem cells relating to bronchial tract. After 3 and 14 days of culture, the cells show growth and proliferation positive toward the study’s overall goal to promote TPU’s use in medicine.

The future of 3D printing in healthcare
The next step for this research, as discussed by Dr. de Mel, is to “discuss regulatory qualifications and relevant ethics to embark on translating pathways” which will in turn bring the application of TPU for elastic tissue into practice.
In our discussion, Dr. de Mel also gave an insight into the future of 3D printing in healthcare. She says,
I envision tissue engineering becoming a point-of-care therapy through the impact of 3D printing. Just as pharmacies are closely linked to hospitals/healthcare units, I believe units for 3D printing (and associated technology) will be closely associated with healthcare centers for tissue replacement or prosthetics.
As previously reported on 3D Printing Industry, such facilities are already becoming a reality, as in the Royal Brisbane and Women’s Hospital in Queensland, Australia. Dr. de Mel continues,
Rapid developments in biomaterials/smart materials should also influence the role of 3D printing in tissue engineering – which means a shift away from traditional sense of tissue engineering; where extensive cell culture procedures are performed on supportive scaffolds to cultivate a tissue in specialized laboratory conditions. Instead, 3D printing will produce biomimetic scaffolds that will prompt the body to act as a bioreactors and encourage in-situ tissue healing and integration.
TPU in wider use
Researchers at Case Western Reserve University (CWRU), Ohio, used TPU in combination with PLA and graphene oxide to create an FDM filament with superior mechanical properties for use in cellular scaffolds. TPU is also used as the bonding layers of MIT’s 3D printed running suit with responsive cooling compartments.
Biomimetic heterogenous elastic tissue development discussed in this article is published in the journal Regenerative Medicine. It is co-authored by Kai Jen Tsai, Simon Dixon, Luke Richard Hale, Arnold Darbyshire, Daniel Martin, and Achala de Mel.
Stay up-to-date with the latest 3D printing research and news by subscribing to our newsletter and following us on twitter and Facebook.
Featured image: SEM image of the internal structure of 3D printed TPU. Image by Dr. Achala de Mel



