Researchers from Tsinghua University, Beijing, have 3D printed a personalized cervix tissue implant to counteract human papillomavirus (HPV). By loading the porous structure of the cone-shaped polyurethane implant with an anti-HPV protein, the team was able to quantitatively control the release of the protein and inhibit HPV growth near the site of the cervix.

HPV and cervical cancer
HPV is the cause of 91% of cervical cancer cases worldwide. With a total of 460,000 new cases annually, the leading treatment is cervical conization, whereby a cone-shaped sample of tissue is removed for diagnostic purposes. The procedure also serves to remove pre-cancerous cells if they are present, and the majority of the tissue grows back within six weeks. The treatment is not a miracle cure, however, as it can lead to tissue defects and tends to see high infection recurrence rates.
3D printed cervix implant
The researchers set out with the aim of developing a non-destructive anti-HPV implant that could also encourage tissue growth at the site of conization. The first step involved designing the conical structure based on medical imaging data – the implant ended up being 30mm in diameter at the base. The material of choice was the FDA-approved implantable biomaterial, polyurethane, and the 3D printing technique employed was low temperature deposition (LDM). Unlike regular FDM, LDM takes place in a sub-zero environment, typically -20°C to -30°C, so phase separation takes place inside the printed structure. Combined with freeze-drying technology, a porous structure can be obtained in the 3D printed part.

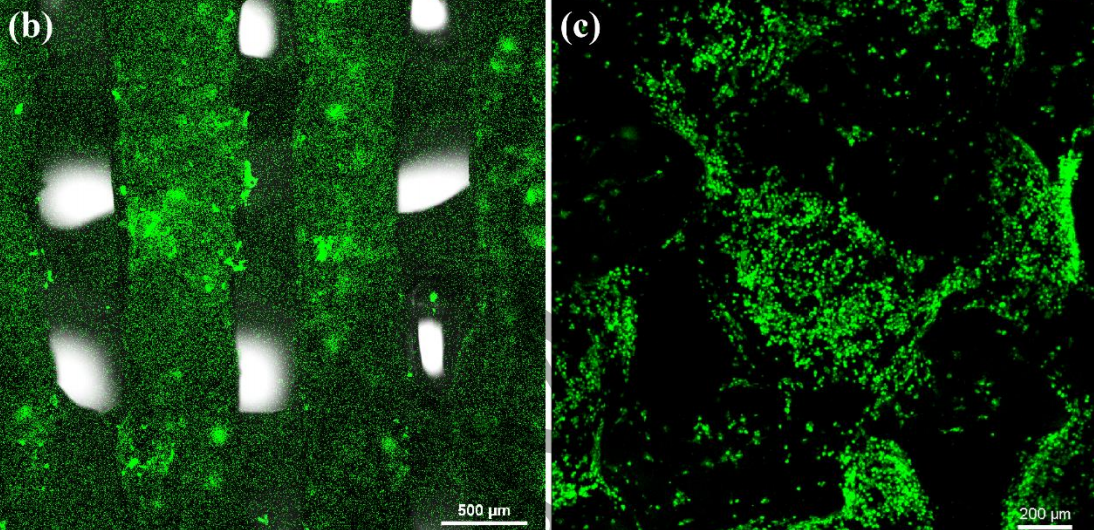
The porosity was important here as it would allow the researchers to load the implant with the anti-HPV ‘JB protein’. To modify and test different porosities, the researchers simply modified their temperature profiles during fabrication and achieved a variety of wire spacings. The team found a linear negative correlation between porosity and protein loading, but the rate of protein release increased with porosity. The protein was found to effectively inhibit HPV from entering host cells and reduced its activity as the site of the implant.
Cytotoxicity and cytocompatibility tests also pointed to the conclusion that the implant encouraged cell growth and adhesion, repairing the healing tissue post-conization. On top of this, the mechanical tests returned mechanical properties comparable to the original cervix tissue – a compressive modulus of 0.06 – 0.25 MPa. The results are a strong indication that 3D printing could be used to repair cervix tissue after conization and inhibit a recurring HPV infection.
Further details of the study can be found in the paper titled ‘Design, modeling and 3D printing of a personalized cervix tissue implant with protein release function’. It is co-authored by Chenjia Zhao, Zitong Wang, Chen Hua, Jingyuan Ji, Zhenzhen Zhou, Yongcong Fang, Ding Weng, Lu Lu, Yuan Pang, and Wei Sun.
3D printed medical implants have featured frequently in AM research over recent months. In April, researchers from Ontario-based Mohawk College and McMaster University became the first to investigate the suitability of a titanium alloy, Ti-5553, for 3D printed bone implants. The cells at the site of the implant displayed extension and growth, suggesting a strong potential for the novel alloy as a bone implant. Elsewhere, at MIT, 3D printing is being used to develop soft, flexible brain electrodes using a conductive polymer liquid material.
The nominations for the 2020 3D Printing Industry Awards are now open. Who do you think should make the shortlists for this year’s show? Have your say now.
Subscribe to the 3D Printing Industry newsletter for the latest news in additive manufacturing. You can also stay connected by following us on Twitter and liking us on Facebook.
Looking for a career in additive manufacturing? Visit 3D Printing Jobs for a selection of roles in the industry.
Featured image shows the porous structure of the implant. Images via Tsinghua University.


