A team from the Wyss Institute for Biologically Inspired Engineering at Harvard University, Massachusetts, have created a 3D printing workflow to predict the performance of artificial heart valves.
A kind of “try before your buy” approach, the researchers have created a software that simulates a valve’s reaction with a patient’s native tissue, and provides accurate medical models specific to each person. In addition, a custom 3D printed “sizer” has been created for a physical demonstration of a valve’s fit.
Together, these features mean surgeons are better prepared to identify risk in relation to a patient’s needs and transcatheter aortic valve replacement (TVAR) operations.
Like shoe shopping…for surgeons
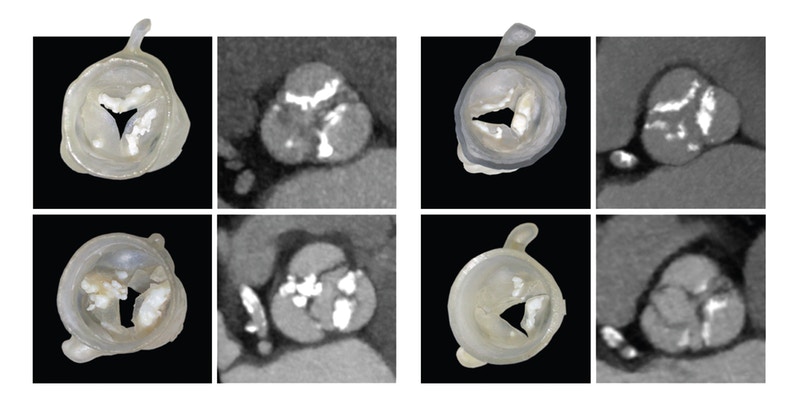
One of the barriers to creating highly accurate, leak-free replacement heart valves is an ability to map the thin “leaflets” of tissue within the thicker walls of a heart’s aorta. In CT scans, these leaflets are faint. However, by identifying seven key points that show up in a CT scan, the Wyss Institute’s software can accurately restructure a patient’s heart valve in its entirety.
After this step a medical model of the patient’s heart, complete with leaflets and any naturally-occuring calcification, is 3D printed using a multimaterial system.
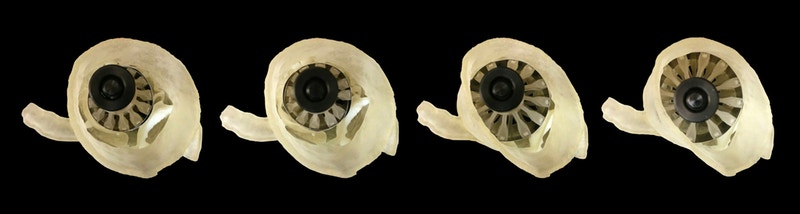
With this physical model, surgeons can then apply the adjustable 3D printed sizer device to determine how an artificial valve would fit inside the natural tissue.
James Weaver, Wyss Institute Senior Research Scientist, likens this process to clothes shopping, “If you buy a pair of shoes online without trying them on first, there’s a good chance they’re not going to fit properly,” he explains.
“Sizing replacement TAVR valves poses a similar problem, in that doctors don’t get the opportunity to evaluate how a specific valve size will fit with a patient’s anatomy before surgery.”
To operate or not to operate?
Putting theory into practice, the team compared predictions from its 3D printed workflow to data from 30 patients who had previously undergone TAVR procedures.
In some of the these cases, leakages had occurred. By applying the sizer and modeling software, the Wyss team proved capable of predicting the rate of leakage in these cases with 60-73% accuracy. This result validated the team’s approach and gave them further areas for future improvement.
Beth Ripley, co-author and collaborator on the Wyss Institute research who was a fellow at Brigham and Women’s Hospital at the time of the study, said, “Being able to identify intermediate- and low-risk patients whose heart valve anatomy gives them a higher probability of complications from TAVR is critical, and we’ve never had a non-invasive way to accurately determine that before.”
“Those patients might be better served by surgery, as the risks of an imperfect TAVR result might outweigh its benefits.”
The results of a study applying this unique method, titled “Pre-procedural fit-testing of TAVR valves using parametric modeling and 3D printing,” have been published online in the Journal of Cardiovascular Computed Tomography. The paper is co-authored by Ahmed Hosny, Joshua D. Dilley, Tatiana Kelil. Moses Mathur, Mason N. Dean, James C. Weaver and Beth Ripley.
2019 3D Printing Industry Awards nominations are now open. Make your selections here.
For progress updates on this project and more from 3D Printing Industry, sign up to our newsletter, follow us on Twitter and like us on Facebook.
Seeking your next opportunity? 3D Printing Jobs is looking for talented candidates like you.
Featured image shows 3D printed medical models of heart valves and varying degrees of calcification. Photo via Wyss Institute at Harvard University


