An interesting medical 3D printing story popped up in Arizona. Researchers from St. Joseph’s Hospital in Phoenix presented some intriguing news at the 2014 Radiological Society of North American (RSNA) meeting. They say that 3D printing is being used in the treatment of aortic stenosis.
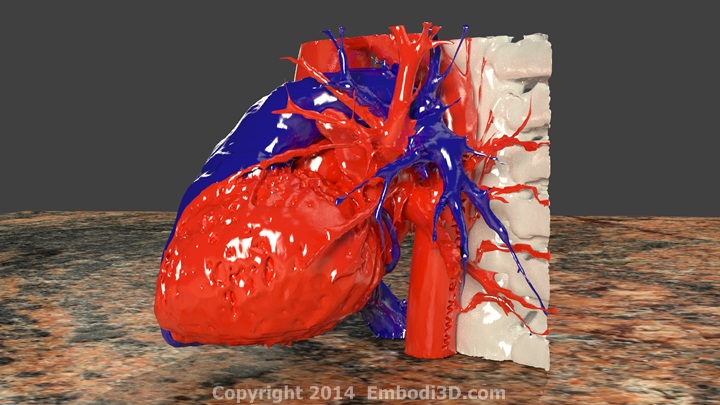
Aortic stenosis occurs when the aortic valve that connects the heart to the aorta does not open correctly. The aortic valve allows blood to be pumped from the heart into the aorta, the main artery of the body. During normal heart contractions, the valve closes to prevent the blood from moving back into the heart. During a heart contraction of a patient with aortic stenosis, the valve doesn’t open, preventing blood from flowing forward. The heart is forced to contract harder and harder to keep blood flowing forward and, over time, severe complications can occur, including fainting, heart failure, heart attack, and even sudden death. Those with severe aortic stenosis who don’t know it, have a 50% chance of dying from it within two years of onset.
Traditional treatments of aortic stenosis include invasive valve replacement surgery. I watched my grandmother recoverfrom this surgery. It is a massive operation, which involves sawing through the breastbone. The factors of risk, complexity, and lengthy recovery times are worrisome by themselves, but they also leave many patients ineligible for such a complex surgery that could potentially save their lives.
There is, however, a new procedure called Transcatheter Aortic Valve Replacement, or TAVR. This involves the implanting of a prosthetic aortic valve. The implantation occurs by navigating the catheter to the heart by inserting it through an artery in the hip. This procedure obviously reduces the invasiveness of surgical treatment. Recovery time significantly drops and patient eligibility spikes.
There is one major problem with TAVR. It requires a highly accurate placement of the prosthetic valve through the catheter, where there is much less room to navigate then, say, if your whole chest is cut wide open. If the valve is the wrong size or is positioned incorrectly, the valve could block the coronary artery, which can potentially form blood clots that lead to stroke. Another complication is the potential tearing of the aorta itself.
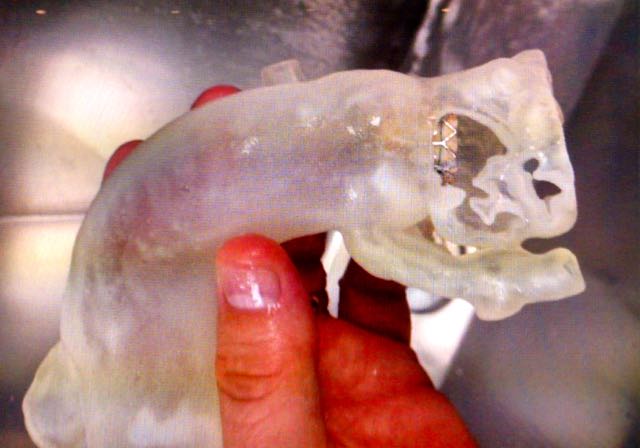
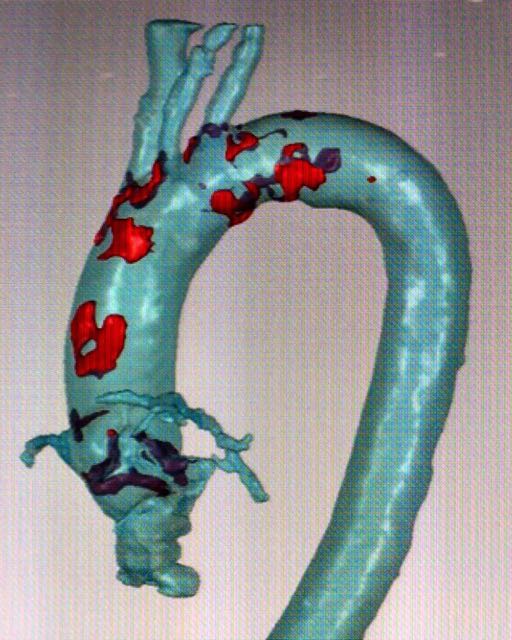
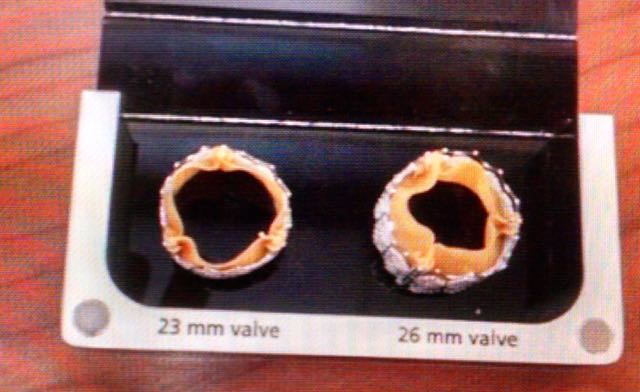
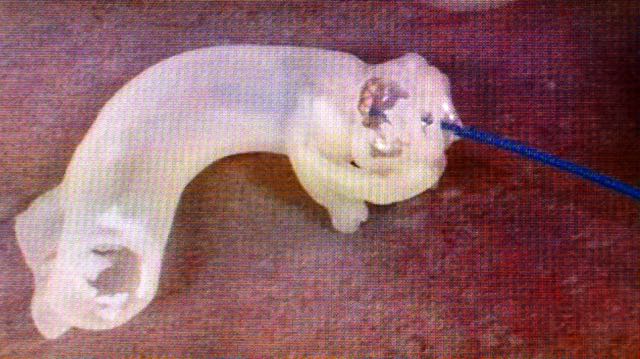
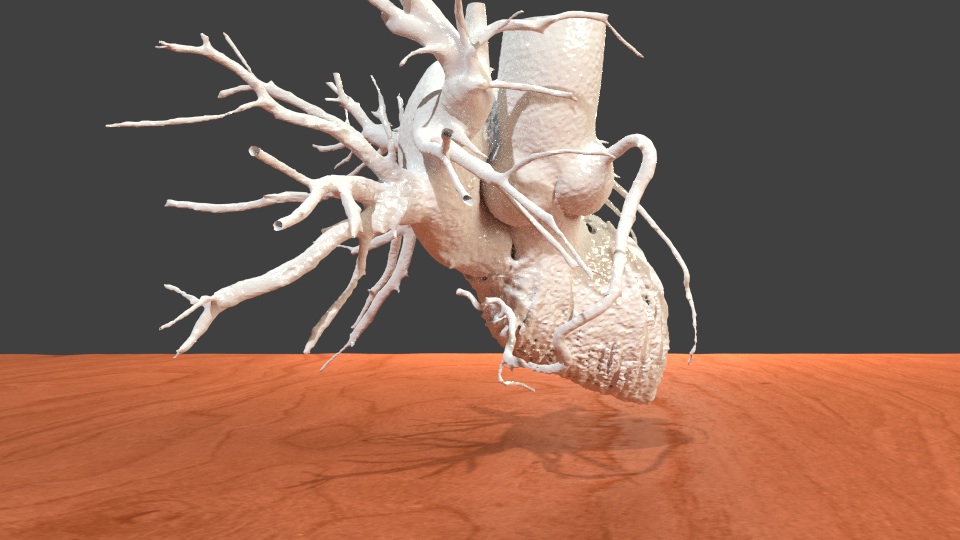
In an attempt to reduce these complications, the St. Johns team implemented what might be called Reality Computing, a term that encompasses 3D scanning, 3D software, and 3D printing as a singular process. The doctors took CT scan data of the hearts, aortas and aortic valves of three patients diagnosed with severe aortic stenosis. With the data, the team 3D printed the aortas and tested various prosthetic valve sizes to see which would fit best.
Next, they CT scanned the prosthetic aortic valves, set them against the scanned heart and aorta data, and compared them to post-op CT scans of patients who had undergone TAVR. They found that the 3D modeled test fitting of the prosthetic valves was very accurate in predicting the performance of the valves in actual patients.
Pre-surgical tests using 3D printed models is proving itself to be one of the most critical medical applications of 3D printing, 3D scanning and 3D software. When all of these tools are used together in one process in medical settings, the results have been overwhelmingly positive for both patients and surgeons. There are some applications that occupy “pivot” zones, where we can expect to see them used similarly in a variety of different ways. What those pivot zones are, we will have to wait and see.