The Mayo Clinic, a non-profit academic medical center based in Rochester, Minnesota, implemented additive manufacturing into its pre-surgical planning processes over ten years ago.
Now, with several successful cases, Dr. Jonathan Morris, Co-Director of the Anatomical Modeling Laboratory and Neuroradiologist at the Mayo Clinic, reflected on the positive impact 3D printed anatomical models have had in addressing unique and complex surgeries.
“3D Printing bridges this gap of taking the unknown and making it known,” said Dr. Morris in a keynote speech at the Materialise World Summit, in Brussels, Belgium.
“The trouble with just having a three-dimensional object on a two-dimensional screen is that it’s still two dimensional. So, if you’re presenting the skull of a two-year-old and an 82-year-old there the same size on the screen – you don’t have any sense of scale.”
Mayo’s Anatomical Modeling Lab
Founded over 150 years ago, the Mayo Clinic, which maintains three campuses across the U.S., treats an estimated 1.3 million patients from 135 countries each year. Within its annual patient treatments, approximately 76,000 surgeries are performed.
Among the vast amount of surgical cases, in 2008, Dr. Christopher Moir, Pediatric Surgeon at the Mayo Clinic, was confronted with five-month-old conjoined twins that were fused at the chest.
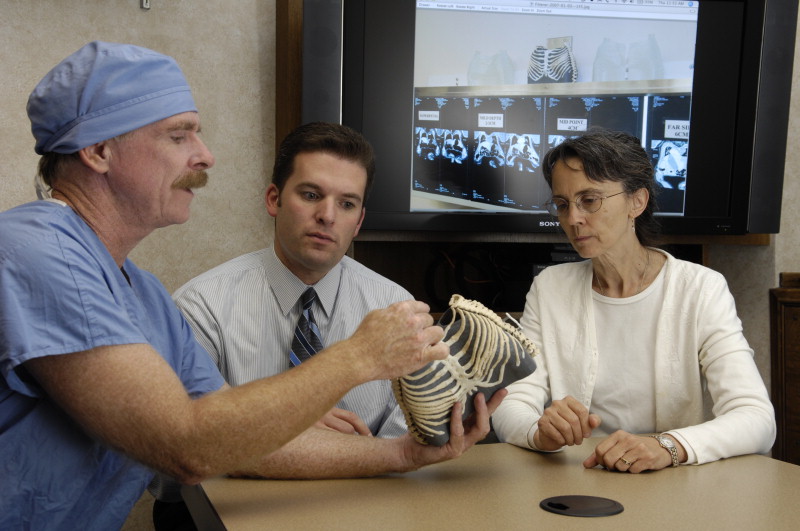
Considering the unusual nature of this case, Dr. Moir and his surgical team sought out Dr. Morris, who had previous 3D printing experience from his time at the National Institutes of Health (NIH), to create customized anatomical models of the twins’ shared organs and rib cage.
These models aided the pediatric team in finding the correct passages and methods to safely separate the twins. In 2016, the widely publicized case of the formerly conjoined Mcdonald twins introduced the capabilities of 3D printed medical models to optimize surgical planning for complex operations. Dr. Morris stated:
“You get an X-ray, CT scan, or an MRI which provides information but until you print that object out and have it in your hands in life-size you’re still in a state of relative uncertainty.”
Following the successful surgical separation of the five-month-old conjoined twins and an influx of similar cases, Dr. Morris and Dr. Jane Matsumoto, Radiologist at the Mayo Clinic, established the Anatomical Modeling Lab.
In-hospital 3D printing
Offering clinical 3D printing services to its three U.S. campuses was not an easy task, explained Dr. Morris. Thus, members of the lab set up a validation workflow, including an ordering system, CAD software (i.e the Materialise Mimics Innovation Suite), and 3D printing systems within Mayo Clinic Operating Rooms (OR).
“[3D printing] has to happen where the doctors are. The fact that it’s in-house makes the lab very accessible for everyone [meaning] surgeons can simply come by between surgeries, explain what they want to visualize, and leave the rest to the radiologists.”
Over the past few years, companies and medical facilities have been integrating additive manufacturing technologies for 3D printing labs within hospitals. Stratasys began installing its Mojo Desktop 3D Printer in five Veterans Affairs (VA) hospitals throughout the U.S. Following this, 3D LifePrints raised £500,000 in Series A funding to expand its medical 3D printing manufacturing operations international level.
With such developments, experienced surgeons and emerging medical practitioners can use 3D printed anatomical models as an education tool within unique and complicated surgical procedures.
Dr. Morris explained,“Surgeons really want to be able to shorten the gap of their trainees to get from knowledge to experience. And 3D Printing does that.”

Catch up with the latest news in 3D printing by subscribing to the 3D Printing Industry newsletter. Also, follow us on Twitter, and like us on Facebook.
Seeking a new position in the additive manufacturing industry? Search and post 3D Printing Jobs for opportunities and new talent across engineering, marketing, sales and more.
Featured image shows Dr. Jonathan Morris giving his keynote presentation at the Materialise World Summit, in Brussels, Belgium. Photo via Materialise.


