Outside of acting as the CEO of Voxel8, Dr. Jennifer Lewis performs cutting edge research into the diverse fields of bioprinting, electronics, and 4D printing, pushing the boundaries of these exciting technologies at every turn. Her most recent breakthrough, with her team at Harvard John A. Paulson School for Engineering and Applied Sciences (SEAS) and the Wyss Institute for Biologically Inspired Engineering at Harvard University, is the 3D printing of thick, vascularized tissues that may have a great deal of significance for the future of artificial tissues and organs.
One of the biggest roadblocks in bioprinting is the ability to 3D print the proper blood vessels for scaling up bioprinted tissues. While we just reported on a story from the University of Toronto, in which blood vessels were created through a stamping process, Prof. Lewis was one of the original pioneers in 3D printing vasculature for delivering nutrients to artificial tissues. This most recent study sees the team build upon this previous work to increase the thickness of their printed tissues by almost ten times through the use of a vascular network, living cells, and an extracellular matrix, resulting in functioning human tissue that can survive for over six weeks.
Published in the Proceedings of the National Academy of Sciences (PNAS), the team’s report details their work in creating complex, thick human tissue containing a network of vasculature for the transmission of fluids, nutrients, and cell growth factors. To do so, Lewis’ team 3D printed a custom, silicone mold consisting of a lattice of vascular plumbing, followed by 3D printed living stem cells.
The structure was then built up, layer by layer, with vertical vascular columns connecting the plumbing throughout the entire object. Once complete, a mixture of fibroblasts and an extracellular matrix is put into the structure, filling all open space and holding the entire structure together.
The resulting print is open at either end, allowing nutrients to flow throughout. Cell growth factors injected into the structure can be carried across the vascular network, as well, encouraging the differentiation of stem cells. Now that the team has invented a process for supporting the blood vessels as the object is fabricated, the shape, thickness, and makeup of the structure can be customized for a given organ tissue.
In the case of this study, Lewis’ group was able to 3D print a one-centimeter-thick tissue made up of human bone marrow stem cells attached to connective tissue and filled with vessels lined with endothelial cells, similar to our own blood vessels. For one month, the team was able to induce the growth of cells in the process of developing into bone cells.
“This latest work extends the capabilities of our multi-material bioprinting platform to thick human tissues, bringing us one step closer to creating architectures for tissue repair and regeneration,” says Dr. Lewis, senior author on the study. David Kolesky, a graduate researcher on the project, adds, “Having the vasculature pre-fabricated within the tissue allows enhanced cell functionality at the deep core of the tissue, and gives us the ability to modulate those cell functions through the use of perfusable substances such as growth factors.”
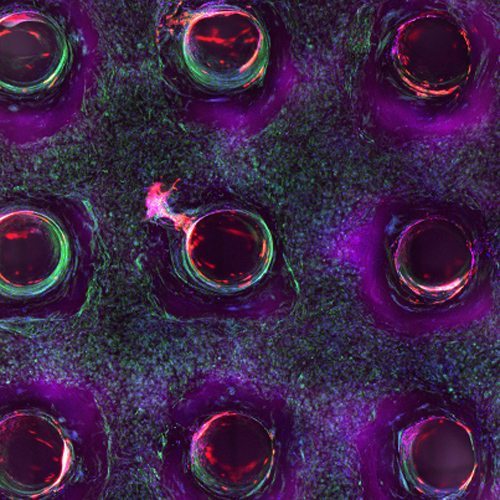
The work of Dr. Lewis’ team goes a long way to developing tissue that could replace animal testing and bring drugs to market much more quickly. Past that, the research could even lead to, one day, complete bioficial organs. But, first, they will have to extend the viability of these 3D printed tissues in order to ensure that the cells can differentiate into their ultimate form.





