3D printing organs and body parts to serve as surgical aids is a trend that has been gathering steam within the industry for some time now. Just last week, 3DPI reported on how doctors in the UK have had the rare opportunity to replicate a brain from London’s Wellcome Collection and use it to aid in training. The Jichi Medical University School of Medicine in Japan have also been using models 3D printed in ABS for neurosurgery classes.
New approaches to the fabrication of surgical models are being tried all the time and Utah based company Whiteclouds have recently launched segmented models of a patient’s MRI as a new method in their 3D-as-a-service business.
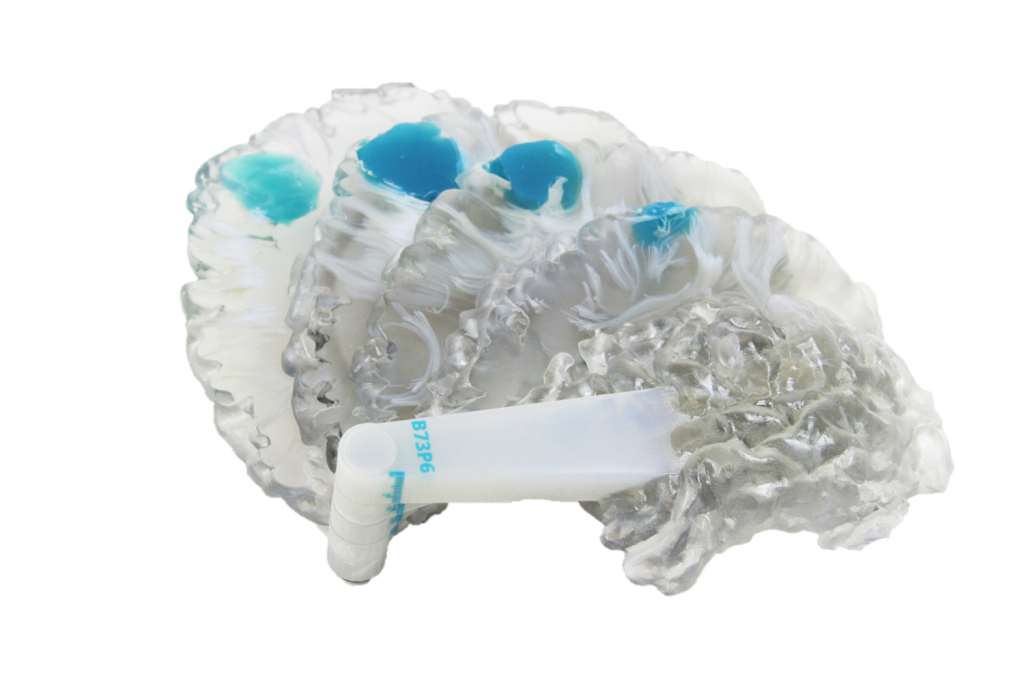
3DPI was eager to discover how valuable these 3D printed models are to the area of neuroscience, and if they really are worth all of this effort. So we asked Dr. Saleem Abdulrauf, a neuroscience expert working with Stratasys Direct Manufacturing, about his experience with the models.
The pros and cons of a simulated brain
To start with, the great thing about 3D printed brains is that they are supported by pre-existing CAT and MRI scan technology. With the aid of these scans, the unique matter, blood vessel and nerve structure of an individual patient’s brain can be recreated with pinpoint accuracy, meaning that a surgeon can learn their way around its physical structure before an operation. It is particularly useful when faced with something like a brain aneurism, as their growth and shape is unpredictable. In these delicate circumstances, surgeons would also want to limit the time taken in theatre, and margin of error as much as possible.
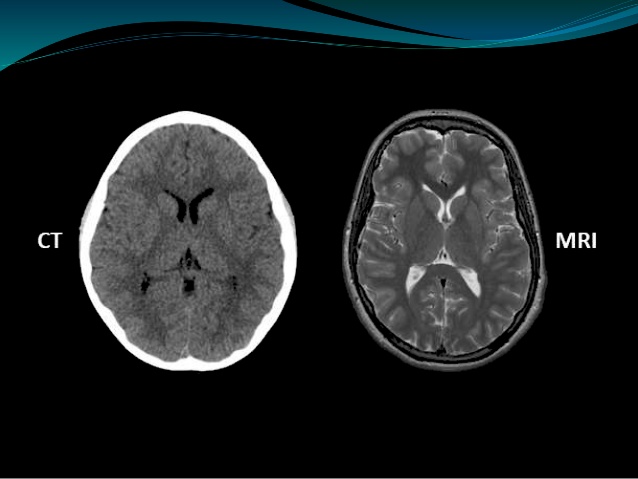
Dr. Abdulrauf says that ‘With [3D] simulation, it makes it a different ballgame which is not fully possible on cadaveric tissue.’ Adding that the downside to using a real brain cadaver is that it isn’t patient specific:
The 3D printed brain is where simulation can take place. With cadavers, we have real structures, but they are not the same as the patient’s aneurysm, tumor, etc. – they are someone else’s, with different branches, characteristics, vessels, etc.
In the physicality of the models, 3D printed brains also have the advantage over digitized brain models as surgeons can practice with the actual tools like they would in theatre, rather than using a cursor in software, or simply studying a 2D image. Both 3D digital models and 2D images are useful for looking at the brain, but neither provide that tactile approach.
Looking to the future
Dr. Abdulrauf went on to say that he and Stratasys are currently testing different materials to 3D print a ‘haptic’ structure of a patient’s brain, where ‘tissue would feel like a real brain does when it’s touched by instruments’.
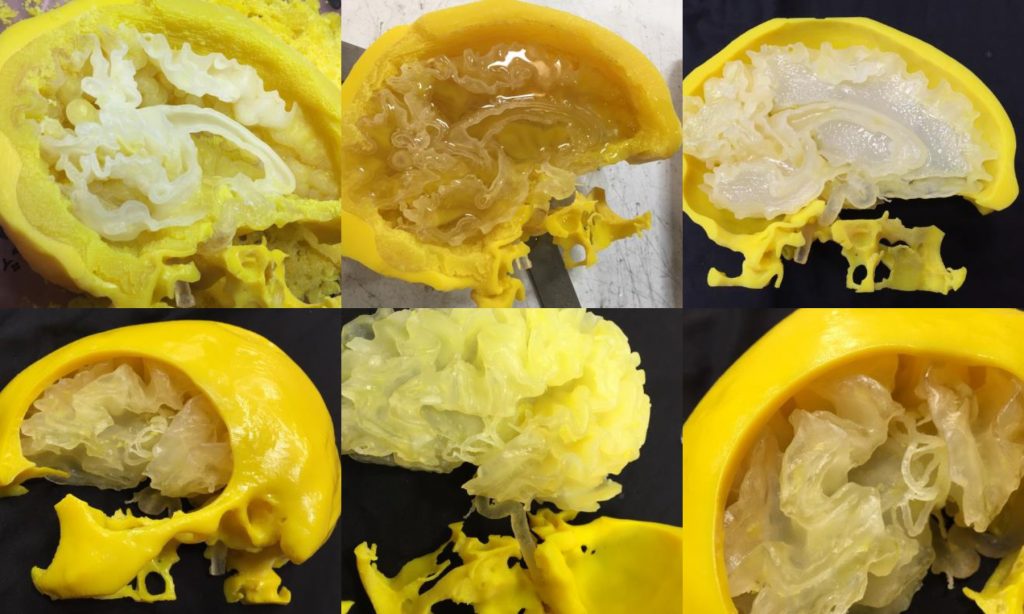
Surgical simulation techniques are also being explored with Microsoft’s new HoloLens hardware, as reported in 3DPI’s article from earlier today. Though neither techniques can ever really standalone as a way of rehearsing surgery, it is exciting that both 3D printing and AI are being used to help one of the world’s most challenging practices. Combining haptic model studies with the 3D printing of living cells may also be some time off yet, but this is valuable groundwork for the future of organs printed for transplants.
Featured image shows a brain MRI scan photograph by Ken Glasercorbis, via: National Geographic


