Researchers at the University of Illinois have 3D printed a miniature microplasma device that could be used to develop more effective antibiotic treatments for middle ear infections.
Designed to be attached to standard clinical otoscopes, the team’s novel microplasma jet array fires charged particles and reactive molecules to disable aural pathogens.
Compared to regular antibiotic treatments, which can cause bacteria to develop defensive ‘biofilms,’ the researchers say their approach provides “increased penetration,” and could even be used as a basis for drug-free remedies moving forwards.
“Biofilms are very dense, making it difficult for the antibiotics to penetrate,” said Helen Nguyen, an Ivan Racheff Professor at the University of Illinois. “We think that microplasma disrupts the biofilm by disturbing the bacterial cell membrane. So far, we only have indirect measurements supporting our idea, but we will look into it in the future.”
“If we can disrupt the structure of [viral] biofilms, we could increase the penetration of antibiotics.”

An antibiotic-free future?
Also known as ‘otitis media’ or ‘OM,’ middle ear infection is a disease prevalent among young kids, which can cause them to suffer a temporary hearing loss that impacts on their early language skills. While antibiotics are often prescribed to treat OM, studies have shown that they’re ineffective in more than 70% of cases, thus the infection has become the leading reason for using general anaesthetic in children.
Chronic cases tend to be related to the build up of a bacterial biofilm in the patient’s middle ear, as their aggregated nature allows them to seed recurrent infections. In order to combat these virulent biofilms, researchers have experimented with microplasma-based approaches in recent years, which have shown particular promise as a means of disrupting pathogens in tight spaces.
In one such test case back in 2018, scientists were able to dramatically reduce the viability of viruses in ten-month-old biofilms, yet their approach hasn’t been applied to OM-related pathogens. To set this right, the Illinois team used 3D printing to create a set of novel microplasma jet array devices, before testing their capabilities by deploying them to ‘treat’ various OM-loaded eardrums models.
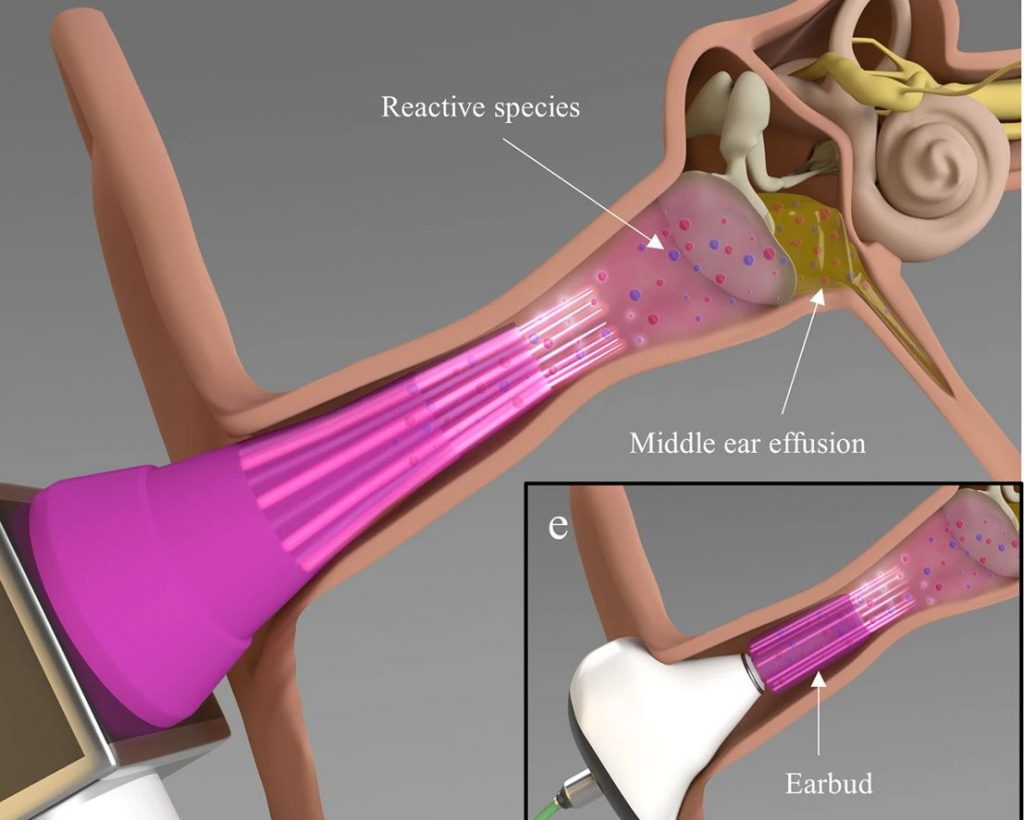
A microplasma jet array in-action
3D printed from clear plastic, each of the scientists’ microplasma devices feature a core frame with an integrated gas input, microchannel diffuser and electrode arrays. During use, the plasmas generated and confined in these microchannel arrays, can theoretically be jetted into the ears of patients on the back of helium, to reduce the viability of aural pathogens.
To put their devices into practise, the researchers used them to treat a resected rat eardrum and chamber, loaded with biofilms housing the common P. aeruginosa bacteria. Initial results showed that after 20 minutes of continuous treatment, the team’s jet array device had managed to clear around 90% of the pathogen, in what constituted the test model’s ‘middle ear’ area.
However, given that rat eardrums are 30% thicker than those of humans, the scientists conducted further testing on a bacteria-loaded artificial membrane that featured a more representative porous structure. This time, the team found “no intact bacterial cells” after treatment, although they did concede that the gas used to carry plasma to their test model, likely disrupted the biofilms’ structure.
Moving forwards, the scientists say that their device requires in-vivo testing to verify their results, thus they’re now developing a more human-friendly earbud-shaped model which should allow for longer exposure times, while they also intend to assess its efficacy at treating other infections like haemophilus influenzae and moraxella catarrhalis.
“As a next step, we will employ a 3D bioprinted eardrum or implantable eardrum scaffolds to examine their structures and properties, including tissue permeability,” concluded the team in their paper. “In-vivo preclinical models, such as OM-induced chinchilla models, would also be helpful to evaluate the efficacy of microplasma on naturally-grown middle ear biofilms.”
3D printing’s aural potential
As the number of antimicrobial 3D printing materials continues to grow, the technology is increasingly being used to treat aural disorders and develop enhanced hearing aid devices. Just last year, scientists at University College London (UCL) 3D printed antibacterial hearing aids that proved capable of preventing ear infections during prolonged use.
Going one step further, researchers at Harvard University’s Wyss Institute have gained FDA approval for their 3D printed ‘PhonoGraft’ regenerating human eardrum. Designed to mimic the appearance of real human aural passages, the eardrum could be used to help treat ear trauma patients, as it’s able to ‘heal itself’ by generating new cells.
On a more commercial level, 3D printer manufacturer Rapid Shape released its Studio-Line HA20 II, HA30 II and HA40 II systems back in 2018. The machines are specifically designed to make 3D printing hearing aids quick and easy to do, while delivering related parts that are both biocompatible and of a professional standard.
The researchers’ findings are detailed in their paper titled “Inactivation and sensitization of Pseudomonas aeruginosa by microplasma jet array for treating otitis media.” The study was co-authored by Peter P. Sun, Jungeun Won, Gabrielle Choo-Kang, Shouyan Li, Wenyuan Chen, Guillermo L. Monroy, Eric J. Chaney, Stephen A. Boppart, J. Gary Eden and Thanh H. Nguyen.
To stay up to date with the latest 3D printing news, don’t forget to subscribe to the 3D Printing Industry newsletter or follow us on Twitter or liking our page on Facebook.
For a deeper-dive into additive manufacturing, you can now subscribe to our Youtube channel, featuring discussion, de-briefs and shots of 3D printing in-action.
Are you looking for a job in the additive manufacturing industry? Visit 3D Printing Jobs for a selection of roles in the industry.
Featured image shows a cutaway view of the team’s 3D printed microplasma jet array device. Image via the biofilms and microbiomes journal.



